For many organizations, returning employees to their worksites has been a journey of one step forward, two steps back. In a current Mercer survey of nearly 800 employers, more than two-thirds (69%) say that new outbreaks of COVID-19 have slowed or halted reopening plans. Still, about half of respondents report that at least 25% of their employees are now at their worksites, and their experience can be used to inform the plans of employers that have not yet reopened worksites.
Back in the spring, there was considerable interest in viral and antibody testing among employers developing worksite return protocols. But survey results show that testing as a requirement for return to work has been largely set aside. In an earlier Mercer survey that closed in July, only 5% of respondents said they required (or planned to require) employees to provide a negative COVID-19 test result before returning to the worksite, and just 2% required or planned to require a positive test for antibodies. Let’s dispense with antibody testing first. While antibody testing, which is performed on blood samples, can tell us who had the virus and may be immune, we still don’t know how effective protection will be and how long it will last, so there’s no guarantee that a person who tests positive for antibodies can’t get sick again or can’t spread the virus. Further, the EEOC issued guidance in June stating that antibody tests may not be required as an obligation for workplace entry.
In terms of testing for the actual virus as a means of preventing outbreaks at the worksite, broad-based testing – that is, testing employees who don’t have symptoms and don’t believe they have been exposed – remains relatively rare. Few employers have opted for universal testing of the workforce – for many, it would be cost-prohibitive– and while testing certain employees on a mandatory basis may be tempting, the EEOC has cautioned that targeted testing of employees raises potential discrimination issues. (The EEOC further states that employers considering diagnostic testing should take steps to ensure the tests are accurate and reliable.)
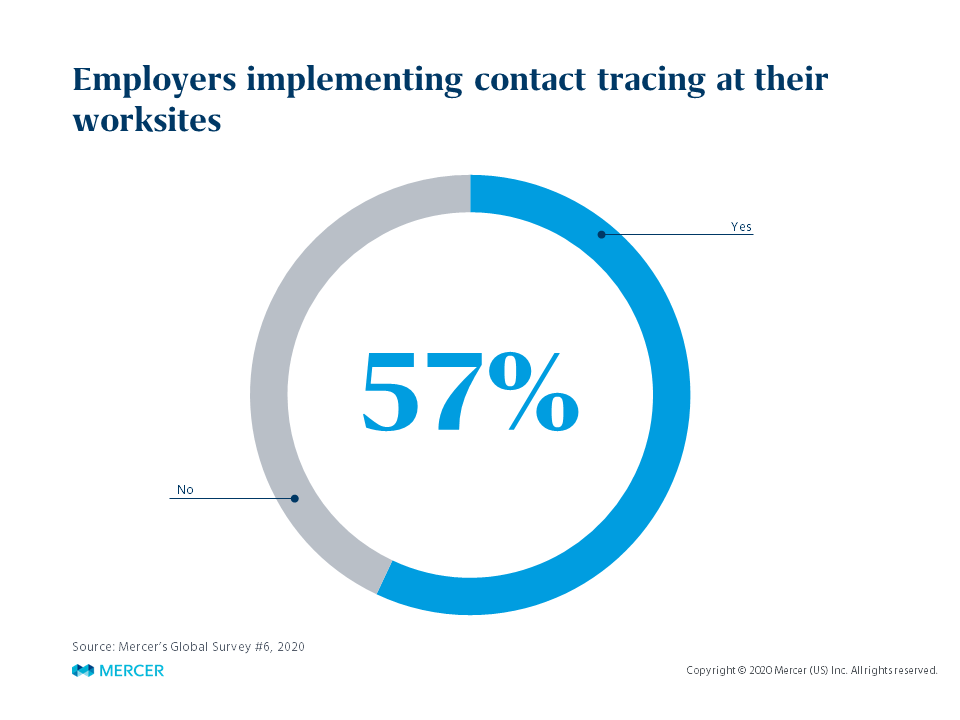
That said, testing for the virus can play an important part of a containment strategy to quickly identify those infected and then proceed with contact tracing – especially important given the likely significant prevalence of asymptomatic and pre-symptomatic spread. Beyond the basics of asking employees about COVID-19 exposure or symptoms,facilitating physical distancing and hand hygiene, and requiring (or encouraging) mask-wearing, contact tracing has emerged as a leading strategy in efforts to keep employees safe at the worksite. Well over half of employers in Mercer’s current survey say they now conduct contact tracing. If you haven’t implemented contact tracing yet, this post by Mercer’s Dr. Dave Zeig is a must-read. As he explains – and illustrates in a handy flow chart -- not only is contact tracing effective, it’s relatively simple to do. On the rocky road to worksite return, “simple and effective” sounds pretty good.